You are here
News
2021
Jul 2021 CRYOLIFE, located in Hong Kong, S.A.R. China, was the first family cord blood bank founded in Asia, 25 years ago. Cryolife is the only private cord blood bank in the world to offer potential clients an option to store their baby's cord blood now and pay two years later.
Jul 2021 Next Biobank (Netcells) has joined hands with the South African Bone Marrow Registry (SABMR) to make cord blood stem cells available to patients in need of a stem cell transplant. Parents that join the "Netcells Community Bank" have their baby’s cord blood HLA typed and listed on a worldwide public registry that can be searched by any patients in need.
Jun 2021 The ideal management of the umbilical cord at the time of birth is still a topic of reseach and controversy. Umbilical cord “milking” describes the practice of manually pushing blood from the umbilical cord into the newborn baby. Cord milking can be an alternative to delayed cord clamping in situations where a delay is not feasible or is not yielding blood transfer. With delayed cord clamping, there is a trade off between allowing cord blood to transfuse into the baby versus being able to collect cord blood for stem cell preservation. With cord milking, there is a risk of causing bleeding in the brains of very premature babies, the same babies that could potentially benefit most from the extra cord blood.
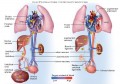
Jun 2021 (1) In late pregnancy, over 450 ml (15 ounces) of blood passes through the placenta per minute.
(2) At birth, a typical umbilical cord holds 60-80 ml (2-2.7 ounces) of blood.
(3) The goal of Delayed Cord Clamping is for some of the cord blood to transfuse into the newborn.
(4) If all the blood in the umbilical cord entered the baby, it would add 20% to the baby’s blood supply.
(5) Delayed Cord Clamping is not possible for all births and does not ensure the infant will receive extra blood.
(6) Full term babies benefit from Delayed Cord Clamping with higher iron levels for up to 6 months.
(7) Premature babies benefit from Delayed Cord Clamping with reduced complications from prematurity.
(8) Delayed Cord Clamping has become the standard of care, but no one agrees how long to delay. MIDWIVES: 2-5 minutes -versus- OBSTETRICIANS: 30-60 seconds
(9) There is a trade-off between Delayed Cord Clamping and collecting umbilical cord blood.
(10) Preserving umbilical cord blood can give lifelong access to stem cells for future medical use.
Jun 2021 Thalassemia is a genetic blood disorder where the body does not properly make hemoglobin, causing chronic anemia. At present the only cure for severe cThalassemia is a stem cell transplant from a matching donor. It was not until the birth of his sister Tahoura, 11 years younger, that Mojtaba was able to have a cord blood transplant that cured his Thalassemia.
May 2021 Cryo-Cell International has obtained exclusive commercial rights to cord blood and cord tissue therapies developed at Duke. Cryo-Cell plans to open infusion clinic(s) that will enable broad public access to any Expanded Access Protocols approved for Duke therapies.
May 2021 Hemocord used the down time of the Coronavirus pandemic to develop and validate new protocols. Hemocord is now licensed by ANVISA for sperm banking. Hemocord has also developed Amnio-Aid, a wound dressing made from amniotic tissue, and has achieved licensing as a Tissue Bank. They are the only laboratory in Brazil that stores amniotic membrane.
Apr 2021 At a time of crisis in South Africa, NEXT Biosciences set up a laboratory to become a COVID PCR testing facility with rapid turn around. Following this two week transformation, requests for help poured in. Soon NEXT Biosciences found themselves setting up and running drive-through testing sites. Hopefully their next challenge will be to operate COVID vaccination sites.
Apr 2021 Immune cell banking could be an insurance policy that helps cancer patients to access personalized immunotherapies like CAR-T therapy. Research suggests that starting CAR-T with better immune cells leads to better patient outcomes, but no study has compared the standard CAR-T protocols to therapies manufactured from previously banked cells. Cord blood banks already have some of the technology and expertise required for immune cell banking.
Mar 2021 Omidubicel is a proprietary stem cell product produced by Gamida Cell that is manufactured from expanded cord blood. Transplants with Omidubicel mimic the short-term advantages of bone marrow but have the long-term benefits of cord blood. In the short term, Omidubicel engrafts faster than a bone marrow transplant. But in the long-term, Omidubicel has the low graft versus host disease of a cord blood transplant. Omidubicel is like a gryphon, a mythical creature with the head and shoulders of an eagle but the hindquarters of a lion.