Usted está aquí
Competing strategies to expand cord blood use for transplants
Today more than 50,000 stem cell transplants are performed annually worldwide, and that number is growing. Only 30% of U.S. patients who need a stem cell transplant can find a suitable donor within their family, while the rest must turn to public registries of bone marrow donors and donated cord blood units. Luckily, cord blood transplants do not have to be as perfectly matched as bone marrow transplants, so they are increasingly used for patients with hard to match genetic types, such as patients of mixed race or of African descent. Cord blood also has the advantage of being ready for immediate use, without spending weeks to months finding and testing potential adult donors. Due to these benefits, more and more physicians are turning to cord blood transplants for treatment of their patients.
Cord blood donations have two big limitations that have kept them from becoming the preferred source for stem cell transplants. One is that there are a limited number of stem cells in a cord blood unit, and often they are not enough for a large adult patient. In recent years transplant centers have worked to overcome this problem by giving patients "double cord" transplants, using two donated cord blood units simultaneously.
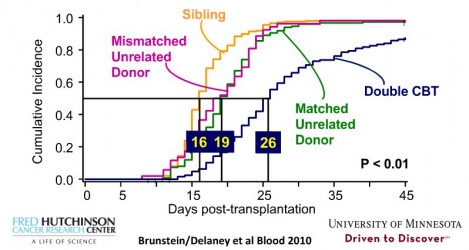
But the other problem is that cord blood does not "engraft" as fast as bone marrow: it takes longer for the patient's immune system to recover. Typical engraftment times are 14 days with bone marrow from an unrelated donor, 16 days with sibling cord blood, and 19 days with cord blood from an unrelated donor (1). Engraftment time is critical because the patient does not have a functioning immune system and is at high risk of a fatal infection during that time window. Simply giving twice as many cord blood stem cells does not speed up engraftment; double cord blood transplants take a median of 26 days to engraft.
Finding ways to speed up cord blood stem cell engraftment has become somewhat of a Holy Grail for the transplant community, both to save patient lives and to increase the utility of banked cord blood. Current research strategies fall into the following three categories:
1. Culture the cord blood stem cells in the lab to "expand" the number of active cells
2. "co-transplant" cord blood stem cells with another stem cell type that will engraft temporarily and act as a bridge until the cord blood stem cells engraft,
3. Enhance the "homing" ability of cord blood stem cells so that they enter the bone marrow faster and engraft.
Figure credit Dr. Colleen Delaney
Below is a table showing some examples (by no means all) of the leading research using these competing strategies:
| Method | Median Engraftment Time | Concept | Proponents (References) |
| Notch-mediated Expansion + Double Cord Transplant | 14 days | Cord blood stem cells are cultured together with recombinant engineered Notch ligand to activate the Notch signaling pathway of cells. The stem cells that test positive for the CD34 assay are multiplied 164 fold. This expanded unit is given with an unmanipulated cord blood unit in a double cord transplant. | Delaney & Fred Hutchinson (2) |
| MSC-mediated Expansion + Double Cord Transplant | 15 days | Cord blood stem cells are cultured together with Mesenchymal Stem Cells (MSC) prior to infusion. The addition of MSC mimics the bone marrow environment so that the Total Nucleated Cell count (TNC) is multiplied 12.2 fold and the CD34 cells are multiplied 30.1 fold. This expanded unit is given with an unmanipulated cord blood unit in a double cord transplant. | Shpall & MD Anderson (3) |
| NiCord Expansion + Double Cord Transplant | 13 days | Using a proprietary method where cord blood stem cells are cultured with nicotinamide, the company Gamida Cell has created a product called NiCord in which the AC133+ cell fraction is enhanced, and the TNC and CD34 cell doses are multiplied 455 fold and 75 fold, respectively. This expanded unit is given with an unmanipulated cord blood unit in a double cord transplant. | Kurtzberg & Duke U. & Gamida Cell (4) |
| Haplo-Cord Transplant | 14 days | Patients receive stem cells from a single cord blood unit that is matched, combined with stem cells from a bone marrow donor who is a half-match (called a haploidentical donor). The half-matched bone marrow engrafts first and acts as a temporary bridge until the matched cord blood engrafts permanently. | Kwon & & U. Gregorio Marañon in Madrid (5) |
| Enhance homing by regulating DPP4 | 21 days | Animal studies show that inhibiting the body's natural dipeptidyl peptidase 4 (aka DPP4 or CD26) allows blood-forming stem cells to engraft faster. Patients receiving single unit cord blood transplants were also given 4 days of oral sitagliptin (aka the diabetes drug Januvia) to inhibit DPP4. The procedure was safe, but the optimum dose for clinical use is still not determined. | Broxmeyer (6,7) |
It is much too soon to speculate as to which of these methods will be widely adopted. If multiple methods achieve the desired engraftment time of 14 days or less, then the next quest will be to discover which strategies are the safest, easiest, and least expensive to implement. We will bring you additional information on these strategies as trials are completed and results are published.
The purpose of Cord Blood Awareness Month is to raise awareness of the use of cord blood and stem cell research that is improving lives daily and will mean so much to our children's future health.
References
- Brunstein, CG et al. 2010 Blood 116(22):4693-4699 (publication)
Allogeneic hematopoietic cell transplantation for hematologic malignancy: relative risks and benefits of double umbilical cord blood - Delaney, C. et al. 2010 Nature Medicine 16:232-236 (press release)
Notch-mediated expansion of human cord blood progenitor cells capable of rapid myeloid reconstitution - De Lima, M. et al. (Shpall) 2012 NEJM 367:2305-15. (news report)
Cord-Blood Engraftment with Ex Vivo Mesenchymal-Cell Coculture - Horwitz, M et al. (Kurtzberg) 2012 BBMT 18(2):S326 (publication)
NiCord® Expanded Hematopoietic Progenitor Cells (HPC) Are Capable of Prolonged Myeloid and Lymphoid Engraftment Following Myeloablative Dual Umbilical Cord Blood (UCB) Transplantation - Kwon, M. et al. 2013 BBMT 19(1): 143-149. (publication & newsletter) Single Cord Blood Combined with HLA-Mismatched Third Party Donor Cells: Comparable Results to Matched Unrelated Donor Transplantation in High-Risk Patients with Hematologic Disorders
- O'Leary, Heather; Ou, Xuan; Broxmeyer, Hal E. April 2013 Current Opinion in Hematology 20:pages doi: 10.1097/MOH.0b013e32836125ac (abstract)
The role of dipeptidyl peptidase 4 in hematopoiesis and transplantation - Farag SS, Srivastava S, Messina-Graham S, et al. (Broxmeyer) 2013 Stem Cells and Development (abstract)
In vivo DPP-4 inhibition to enhance engraftment of single-unit cord blood transplants in adults with hematological malignancies.